RESEARCH ARTICLE | https://doi.org/10.5005/jp-journals-10005-1976 |
Assessing the Pain Reaction of Children and Evaluation of Efficacy of Buccal Infiltration with Articaine and Inferior Alveolar Nerve Block with Lignocaine for Pulp Therapy in Primary Mandibular Second Molars
1–4Department of Pedodontics and Preventive Dentistry, Mamata Dental College, Khammam, Telangana, India
Corresponding Author: Velagala Daneswari, Department of Pedodontics and Preventive Dentistry, Mamata Dental College, Khammam, Telangana, India, Phone: +91 7569890870, e-mail: dollypedo@rediffmail.com
How to cite this article Daneswari V, Venugopal Reddy N, Madhavi G, et al. Assessing the Pain Reaction of Children and Evaluation of Efficacy of Buccal Infiltration with Articaine and Inferior Alveolar Nerve Block with Lignocaine for Pulp Therapy in Primary Mandibular Second Molars. Int J Clin Pediatr Dent 2021;14(3):335–339.
Source of support: Nil
Conflict of interest: None
ABSTRACT
Introduction: Pain-free operating is of obvious benefit to the patient, it also helps the operator as treatment can be performed in a calm, unhurried fashion. Articaine hydrochloride has steadily grown in popularity, and studies have shown that articaine hydrochloride performs better than lidocaine due to an enhanced anesthetic efficacy.
Aim and objective: To assess the efficacy of buccal infiltration with articaine in achieving anesthesia for pulp therapy in primary mandibular second molars as compared with inferior alveolar nerve block (IANB) with lignocaine.
Materials and methods: Thirty patients (4–8 years) with an indication of pulp therapy in at least two primary mandibular second molars were selected. Patients were randomly assigned to receive nerve block with lignocaine on the first appointment and buccal infiltration with articaine on the second appointment spaced 1 week apart. A single researcher injected local anesthetic for all the patients. Two researchers standing at a distance of 1.5 m recorded the pain scores and sound, eye, motor (SEM) scores. After the completion of the procedure, the patient was asked to record facial image (FI) score and Heft-Parker visual analog score (HP-VAS).
Results: The pain-related behavior scores were higher for IANB when compared with infiltration. Facial image and HP-VAS scores were higher for the lignocaine IANB group when compared with the articaine infiltration.
Conclusion: With the increasing use of new delivery systems such as single tooth analgesia, a buccal infiltration with articaine provides an effective alternative, with minimal discomfort which would allow clinicians to avoid the use of IANB in children.
Keywords: Articaine, Buccal infiltration, Inferior alveolar nerve block, Lignocaine, Primary second molars.
INTRODUCTION
Pain-free surgery is obviously beneficial to the patient, but it also benefits the operator because treatment can be done in a relaxed, unhurried manner.1 Many adults have developed a strong aversion to dental treatment as a result of negative childhood experiences.2 Disposable cartridges, traditional methods of infiltration, or nerve block treatments with a dental syringe needle are used in the majority of local anesthetic treatments in pediatric dentistry, as documented so far. Alternative methods, on the other hand, are available such as computer-controlled local anesthetic distribution, periodontal injection techniques (i.e., PDL, intraligamentary, and peridental injection), needleless systems, and intraseptal or intrapulpal injection are among them.3
While treating primary molars, maxillary infiltration and mandibular nerve block are the preferable procedures for achieving local anesthesia.4 Despite the fact that these local anesthetics have a long history of efficacy and safety, they all can trigger substantial toxicity.5
Mandibular nerve blocks employing the Gow-Gates technique and Akinosi technique have been offered as options for inferior alveolar nerve block (IANB); however, they have been proven to be technically more difficult and associated with numerous problems such as hematoma and post-injection trismus.6
The potency and diffusion capacities of a local anesthetic drug may influence infiltration efficacy. As a result, another element to consider was the type of local anesthetic used. Since Malamed’s anesthetic reports in 1986 revealed that articaine hydrochloride had 1.5 times the potency of lidocaine, it was thought that the higher potency would result in improved infiltration.7 Local anesthetics have made significant progress in dentistry and have significantly altered patient perceptions of dental treatments. There is still room for painless procedures for administering local anesthetics to be developed. To take advantage of all of the local anesthetic devices and techniques available for dental operations, physicians must be well-versed in them.2 Articaine hydrochloride has steadily gained popularity, and tests have shown that it performs better than lidocaine due to improved anesthetic efficacy.8 There have been very few clinical trials that have shown that articaine is superior to lignocaine.9 As a result, the purpose of this study was to compare the efficacy of buccal infiltration with articaine against IANB with lignocaine in obtaining anesthesia for pulp treatment in primary mandibular second molars.
PATIENTS AND METHODS
Thirty patients in the age range of 4–8 years, 13 males and 17 females, were selected from Mamata Dental College and Hospital’s outpatient department in Khammam, India. Frankl’s behavior ratings III and IV, an indication of pulp therapy in two primary mandibular second teeth, patients were chosen based on the lack of soft tissue lesions at the injection site and no history of local anesthetic solution allergy. Informed consent from the parents was obtained before recruiting the patients for the study. Approval to conduct this study was obtained from the institutional ethical clearance committee of Mamata Dental College and Hospital, Khammam.
This research used a crossover design, in which both injection procedures were used in the same patient for pulpotomy of two primary mandibular second molars across two 1-week appointments. Benzocaine gel was first applied to the injection site. On the first appointment, patients were randomly assigned to receive IANB with 1.8 mL of 2% lignocaine hydrochloride and 1:80,000 adrenaline solution (Xicaine, ICPA) and buccal infiltration with 0.8 mL of 4% articaine hydrochloride and 1:100,000 epinephrine (Septocaine, Septodont) on the second appointment. The local anesthetic was injected by a single researcher for all of the patients. After loading the injections with the appropriate amount of local anesthetic agent, 2 mL disposable syringes with 25-gauge needles were used to deliver the injections. A rubber dam was used to isolate the selected teeth under local anesthesia. Before the pulp was exposed, the cavity outline shape was established and all marginal caries were eliminated. The coronal pulp was exposed using a sterile number 6 carbide round bur. The access cavity was enlarged to the limit of the pulp horns to simplify coronal pulp excavation. With the help of a sterile sharp spoon excavator, the coronal pulp was amputated. To avoid dentinal chips from being driven into the radicular pulp, the pulp chamber was irrigated with sterile saline. After irrigation, sterile cotton pellets were placed on the severed pulp stumps to aid in hemostasis. After this standardized technique, the quality and the quantity of blood from the exposure site have got diagnostic importance. On the pulp stumps, a cotton pellet moistened with formocresol for 1 minute was inserted. The cavity was rinsed with normal saline after the pellet was removed. Over the dressed pulp stumps, a layer of reinforced zinc oxide eugenol was placed (Fig. 1). All the pulp therapy procedures for every patient were performed by the same operator on both appointments.
The pain scores and sound, eye, and motor (SEM) scores were recorded by two researchers standing 1.5 ms apart. The scores were calibrated by the second observer, and the first observer’s values were used for statistical analysis. The pain score is given by Ram and Peretz10 (Table 1) was used to evaluate pain during injection, and the SEM score7 (Table 2) was used to evaluate pain during access opening and extirpation of the pulp. Patients self-assessed their experience after the surgery by recording their facial image (FI) score (Fig. 2) and Heft-Parker Visual Analog Score (HP-VAS) (Fig. 3). Because both injection procedures were distinct and detectable, blinding was not possible in this research. The data were generated and statistical analysis was performed using SPSS version 16.0. The Mann–Whitney U test was used to make comparisons between the two procedures.
RESULTS
Thirty individuals (17 females, 13 males) with an average age of 5.41 ± 1.40 years were included in the study (range 4–8 years).
Evaluation of Pain on Injection
The various parameters for pain score are shown in Table 1. When IANB administration was compared to infiltration, the eye squeezing ratings (p 0.001), hand movement (p 0.001), and leg movement (p 0.05) were considerably greater, but the differences in the scores for torso movement and crying were not statistically significant. Thus, the pain-related behavior scores were higher for IANB when compared with infiltration.
Evaluation of Pain during Pulp Extirpation
ANOVA was used to do statistical analysis on SEM scores, followed by the determination of the Mann–Whitney U value. The SEM scores for age and sex-based mean values are shown in Table 3. The findings revealed that the ratings for IANB were significantly higher than infiltration for both sexes and age groups, implying that IANB failed to produce enough pulp anesthesia in some circumstances.
Evaluation of Overall Experience of the Patient
The mean values for the FI and HP-VAS scores are included in Tables 4 and 5, respectively. The findings of the Mann–Whitney test showed that the lignocaine IANB group had higher scores than the articaine infiltration group, implying that the patients with articaine infiltration had a better overall experience.
DISCUSSION
One of the most significant challenges in providing dental care to children is anxiety. Injection seems to be the procedure that causes the most anxiety in both children and adults. Local anesthetic is both the savior and the bane of modern dentistry, which is ironic. It allows for nearly painless treatment, but it is also linked to a lot of anxiety and misunderstandings among young patients.10 Newer technologies have been developed to help dentists provide improved pain management with less injection pain and minimal adverse effects. Knowledge of the agents being used, the neuroanatomy involved, and the best techniques and devices available are all required for good local anesthesia.2 During the propagation of the action potential, articaine reversibly prevents the conduction of nerve impulses by inhibiting the sodium and potassium channels. Articaine has a half-life of roughly 20 minutes in the body.11
Although there are certain drawbacks to using articaine in the mouth, avoiding IANBs for restorative dentistry has several benefits. For less invasive operations, infiltration reduces unwanted soft-tissue anesthetic, requiring an additional injection for lingual anesthetic. In mandibular molar anesthesia, buccal infiltration with articaine has been proven to have a greater success rate than buccal infiltration with 2% lidocaine and epinephrine (1:100,000). This improvement in efficacy could be due to a concentration effect or increased articaine diffusion. If the buccal dose is decreased to a “critical” level, lingual infiltration may become important.12 Because nerves emerging from inflamed tissue have altered resting potentials and lower excitability thresholds, teeth with irreversible pulpitis (IP) are perceived to be more difficult to anesthetize than teeth with normal pulp.13

Fig. 1: Lignocaine (pulpotomy irreversible pulpititis 75), Articaine (pulpotomy irreversible pulpititis 85)
| IANB lignocaine | Infiltration articaine | Chi-square statistic | |
|---|---|---|---|
| Eye squeezing | 22 | 6 | p %3C; 0.001** |
| Hand movement | 14 | 2 | p < 0.001** |
| Torso movement | 4 | 1 | p %3E; 0.05 |
| Leg movement | 7 | 0 | p > 0.05* |
| Crying | 6 | 1 | p > 0.05 |
* Significant
** Highly significant
| Parameter | Comfort | Mild discomfort | Moderate discomfort | Severe discomfort |
|---|---|---|---|---|
| Grade | I | II | III | IV |
| Sound | No sound | Non-specific sound (probable pain) | Verbal complaint, louder sound | Verbal complaint, shouting, crying |
| Eye | No sign | Dilated eye without a tear (anxiety sign) | Tears, sudden eye movements | Crying, tears all over the face |
| Motor | Relaxed body and hand status | Muscular contraction, contraction of hands | Sudden body and hand movements | Hand movements for defense, turning the head to the opposite side |
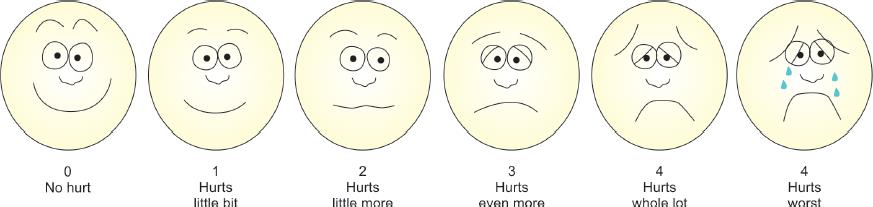
Fig. 2: Facial image score
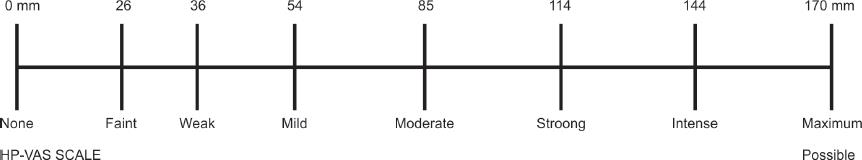
Fig. 3: HP-VAS score
| Males (N = 13) | Females (N = 17) | Age-group. 4–5 years (N = 14) | Age-group. 6–8 years (N = 16) | Total (N = 30) | |||||
|---|---|---|---|---|---|---|---|---|---|
| Mean score | Mann–Whitney statistic | Mean score | Mann–Whitney statistic | Mean score | Mann–Whitney statistic | Mean score | Mann–Whitney statistic | Mann-Whitney statistic | |
| IANB lignocaine | 5.13 | p < 0.01 | 5.35 | p < 0.001 | 5.69 | p < 0.001 | 4.8 | p < 0.05 | p < 0.001 |
| Infiltration articaine | 3.34 | 3 | 3.3 | 3.5 | |||||
* Significant
** Highly significant
| Males (n = 17) | Females (n = 13) | Age 4–5 years (n = 14) | Age 6–8 years (n = 16) | Total (n = 30) | |||||
|---|---|---|---|---|---|---|---|---|---|
| Mean score | Mann–Whitney statistic | Mean score | Mann–Whitney statistic | Mean score | Mann–Whitney statistic | Mean score | Mann–Whitney statistic | Mann–Whitney statistic | |
| IANB lignocaine | 1.13 | p < 0.01 | 1.02 | p < 0.01 | 5.68 | p < 0.001** | 1.03 | p < 0.01 | p < 0.001 |
| Infiltration articaine | 0.16 | 0.18 | 3.15 | 0.05 | |||||
* Significant
** Highly significant
In the case of a painful endodontic emergency, an effective local anesthetic is essential. Because of local acidosis generated by tissue inflammation and inflammatory mediator activation of nociceptors, the success rate of anesthesia in patients with permanent pulpitis may drop dramatically.9 A mechanical mouth prop was utilized to deliver the mandibular block, which required the youngster to open his mouth as wide as possible. The ball of the thumb was placed on the coronoid notch of the anterior border of the ramus, and the fingers were placed on the posterior border of the ramus. The needle was gently placed between the internal oblique ridge and the pterygomandibular raphe. After negative aspiration, a small amount of solution was injected, and the needle was gently and slowly advanced. After that, the long buccal nerve was anesthetized. A rubber dam was used for all of the operational procedures. Both infiltration and mandibular block were performed with a short needle (20 mm, 25 gauge). The injection of the local anesthetic was slow, taking nearly two minutes on average for around 1 mL each minute.10
| Males (n = 17) | Females (n = 13) | Age 4–5 years (n = 14) | Age 6–8 years (n = 16) | Total (n = 30) | |||||
|---|---|---|---|---|---|---|---|---|---|
| Mean score | Mann–Whitney statistic | Mean score | Mann–Whitney Statistic | Mean score | Mann–Whitney statistic | Mean score | Mann–Whitney statistic | Mann–Whitney statistic | |
| IANB lignocaine | 28.10 | p < 0.01 | 19.65 | p < 0.01 | 20.15 | p < 0.001 | 23.8 | p < 0.01 | p < 0.001* |
| Infiltration articaine | 7.05 | 3.5 | 1.63 | 8.07 | |||||
* Significant
** Highly significant
Because it is believed that pain is caused, at least in part, by the volume pressure changes produced by the injected fluid on tiny nerve fibers, a longer injection time has been studied as a means of minimizing the pain associated with an injection. One way to control the volume pressure is to slow down the pace of administration.14 Infiltration with articaine has recently been found to be an efficient method of obtaining anesthetic for mandibular molars. In our current investigation, we discovered that IANB with lignocaine and articaine had similar efficacy, but that infiltration with articaine achieves a better anesthetic than infiltration with lignocaine.6 While comparing buccal infiltration with articaine to IANB with articaine, Jung et al. discovered that buccal infiltration with articaine had a faster onset and equivalent efficacy.15
Articaine infiltration was found to be just as effective as lignocaine IANB for pulpal anesthesia in mandibular primary molars in the present study. In a comparable study, articaine infiltration was found to be as efficient as lignocaine IANB for pulpal anesthetic in permanent mandibular teeth by Corbett et al.12 As evidenced by ocular squeezing and muscular contraction, discomfort on IANB was significantly greater than infiltration in this study. Because of the increased volume and duration of injection, Sharaf determined that nerve block is more painful than local infiltration.6
In the present study, it was discovered that infiltration with articaine produced better anesthesia than IANB with lignocaine, which was in agreement with a study conducted by Alzahrani et al., who reported that the local anesthetic efficacy of 4% articaine hydrochloride used as buccal infiltration with intrapapillary infiltration and 2% lidocaine hydrochloride used as IANB were both equally successful.8
Inferior alveolar nerve block had lower HP-VAS and FI scores than infiltration, which can be explained by a combination of variables such as initial discomfort on injection and failure to attain pulpal anesthesia. As a result, children tolerated articaine infiltration better than IANB with lignocaine. Infiltration would also benefit children with special health care needs, such as coagulation abnormalities because it can be administered without the need for replacement therapy.6 Not only is an IANB more painful than a BI, but it also has a higher risk of complications like trismus and hemorrhage.8
Although no side effects were identified with articaine except for the prolonged soft tissue anesthetic that lasted for up to 2–4 hours in our current trial, 20% of the 4–8-year-old suffered soft tissue injuries. With the growing use of novel delivery systems like single tooth analgesia, a buccal infiltration with articaine offers a viable alternative with minimal discomfort, allowing practitioners to avoid using IANB in children.8 To ensure the safety of children, more studies with a larger sample size are recommended.
REFERENCES
1. Meechan JG. How to overcome failed local anaesthesia. Br Dent J 1999;186(1):15–20. DOI: 10.1038/sj.bdj.4800006.
2. Saxena P, Gupta SK, Newaskar V, et al. Advances in dental local anaesthesia techniques and devices: an update. Natl J Maxillofac Surg 2013;4(1):19–24. DOI: 10.4103/0975-5950.117873.
3. Guideline on use of local anesthesia for pediatric dental patients. AAPD 2015.
4. Yilmaz Y, Eyuboglu O, Keles S. Comparison of the efficacy of articaine and prilocaine local anaesthesia for pulpotomy of maxillary and mandibular primary molars. Eur J Paediatr Dent 2011;12(2):117–122.
5. Baroni DB, Franz-Montan M, Cogo K, et al. Effect of articaine on mental nerve anterior portion: histological analysis in rats. Acta Odontol Scand 2013;71(1):82–87. DOI: 10.3109/00016357.2011.654243.
6. Chopra R, Marwaha M, Bansal K, et al. Evaluation of buccal infiltration with articaine and inferior alveolar nerve block with lignocaine for pulp therapy in mandibular primary molars. J Clin Pediatr Dent 2016;40(4):301–305. DOI: 10.17796/1053-4628-40.4.301.
7. Wright GZ, Weinberger SJ, Marti R, et al. The effectiveness of infiltration anaesthesia in the mandibular primary molar region. Pediatr Dent 1991;13(5):278–283.
8. Alzahrani F, Duggal MS, Munyombwe T, et al. Anaesthetic efficacy of 4% articaine and 2% lidocaine for extraction and pulpotomy of mandibular primary molars: an equivalence parallel prospective randomized controlled trial. Int J Pediatr Dent 2018;28(3):335–344. DOI: 10.1111/ipd.12361.
9. Ali SG, Mulay S. Articaine vs lidocaine: a review. IOSR-JDMS 2014;13(9):40–44. DOI: 10.9790/0853-13954044.
10. Ram D, Peretz B. Reactions of children to maxillary infiltration and mandibular block injections. Pediatr Dent 2001;23(4):343–346.
11. Adewumi A, Hall M, Guelmann M, et al. The incidence of adverse reactions following 4% septocaine (articaine) in children. Pediatr Dent 2008;30(5):424–428.
12. Corbett IP, Kanaa MD, Whitworth JM, et al. Articaine infiltration for anesthesia of mandibular first molars. J Endod 2008;34(5):514–518. DOI: 10.1016/j.joen.2008.02.042.
13. Yapp KE, Hopcraft MS, Parashos P. Articaine: a review of the literature. Br Dent J 2001;210(7):323–329. DOI: 10.1038/sj.bdj.2011.240.
14. Allen KD, Kotil D, Larzelere RE, et al. Comparison of a computerized anaesthesia device with a traditional syringe in preschool children. Pediatr Dent 2001;24(4):315–320.
15. Jung IY, Kim JH, Kim ES, et al. An evaluation of buccal infiltrations and inferior alveolar nerve blocks in pulpal anesthesia for mandibular first molars. J Endod 2008;34(1):11–13. DOI: 10.1016/j.joen.2007.09.006.
________________________
© The Author(s). 2021 Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (https://creativecommons.org/licenses/by-nc/4.0/), which permits unrestricted use, distribution, and non-commercial reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data made available in this article, unless otherwise stated.